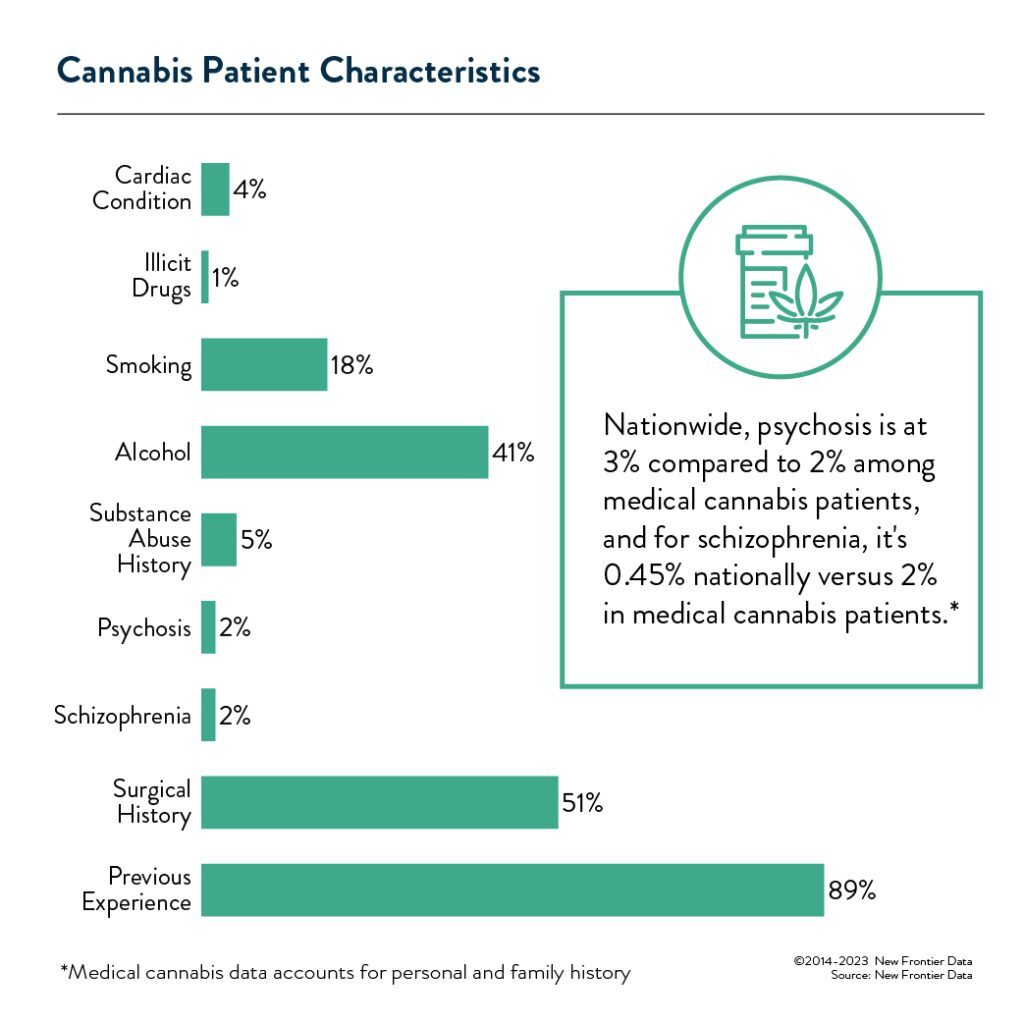
Unique challenges for the medical side of cannabis

Cannabis consumers in 2022 vs. 2023: The evolution of mainstreaming
September 19, 2023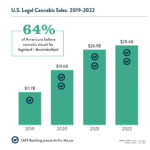
Safety in Numbers
October 17, 2023By Dr. Amanda Reiman (Ph.D., MSW), Chief Knowledge Officer, New Frontier Data
Last week, the Cannabis Science Conference took place in Providence, Rhode Island. Unlike the bevy of conferences focused on growing the industry, this was a chance for researchers and patient advocates to review the latest in medical cannabis research. It was also a chance to discuss the impact that the recreational side is having on those who use cannabis as medicine. It is true that over half of cannabis consumers report their use to be both medical and recreational. However, as the stigma around cannabis lessens, as more medical professionals become versed in its use as a medicine and more states introduce medical cannabis programs, there is an influx of consumers who fall strictly on the medical side. According to the 2023 Consumer Survey from New Frontier Data, medical-specific consumer groups like Medical Lifestylers and Modern Medicinals are growing, while traditionally recreational leaning groups like Savvy Connoisseurs are shrinking. Furthermore, when asking non-consumers about the circumstances under which they would try cannabis, the most popular answers were if they were diagnosed with a medical condition for which cannabis could be useful and if their doctor recommended it. This conference was a chance to better understand the challenges facing consumers who are using cannabis solely as medicine.
Lack of variety in product choice at the dispensary
While some medical patients are seeking high THC flower, they are more likely than recreational consumers to use lower potency products, to seek products with a complex cannabinoid profile, and to choose forms like tinctures and topicals. These products can be hard to find in a sea of 30% THC prerolls and high-potency concentrates. Additionally, products preferred and recommended by budtenders may not be desired or appropriate for those just getting into cannabis as a therapeutic tool. Notable at the conference were the number of nurses and others who work with patients, sometimes reviewing dispensary menus together, to identify products that will meet their needs.
Lack of medical professionals willing to discuss and recommend cannabis
While there is a growing number of medical professionals willing to consider cannabis as a medical treatment, those with enough knowledge to properly consult with a patient and recommend various treatment paths are still rare. Furthermore, these doctors are usually not primary care physicians or mental health professionals, but rather they exist outside of the patient’s treatment ecosystem. This can lead to fragmented care and the patient having to avoid talking about their medical cannabis use with their health professional. And, since there are real medication interactions to consider, this leaves the patient in a precarious place. Much of the conversation at the conference was around how to get more mainstream physicians and psychiatrists on board with medical cannabis to help streamline and strengthen the continuum of care.
Cost and research barriers to using cannabis in a harm reduction context
One theme of the conference was the benefit of using cannabis as an adjunct to other medications like opiates that carry with them a greater level of potential harm. The barrier here, besides physician acceptance of cannabis, is the current federal framework. And while the move to Schedule III was touched on, the bigger conversation was around insurance reimbursement. The difference between paying $15 a month for opiates or Benzo’s, and $100 a month for medical cannabis is most felt by those who are economically vulnerable. As a result, they end up being pushed towards medications with a higher risk of dependence and overdose. And even though the funding for medical cannabis research has improved in the past few decades, the Schedule I status still relegates studies to animal models and small sample sizes.
To this last point, New Frontier Data, in partnership with CMED Data, now has a database of over 150K patients and growing. This data covers demographics, medical history, current cannabis use patterns, and standardized assessments of pain, anxiety, insomnia, physical functioning, nausea, and PTSD. All data have been de-identified and can be used for analysis. We can also recruit from this sample for specific research questions posed by academic researchers, government researchers, regulators and others. This is an opportunity to learn more about medical cannabis patients and how their health changes after becoming patients. We hope that this resource will move the needle on medical cannabis patient research and will lead to a greater acceptance of cannabis as medicine, policies that support it as a front-line therapy, and a retail market that reflects the needs of this growing group of consumers.